Working in a histology lab means that I get to see a lot of what our body looks like under the microscope. Quarterly I will share with you some of my photos from the microscopic world of our inner space and tell you a little bit about what we’re looking at.
This quarter we focus on one of the most common surgical specimens received in the lab; the haemorrhoid.
Despite being a very common ailment of the anal canal, particularly for people in their 40s, their aetiology is still debated. Some thoughts on causes include:
- Loosening of the mucosal attachment to the outer bowel wall causing prolapse and tightening of the anal canal. This compresses the cushion and causes congestion and dilation of blood vessels.
- An age-related fibrotic change of the tissue that is connected to the internal sphincter and longitudinal muscles, which causes tightening of the anus and subsequent prolapse.
- Neuronal hyperplasia or changes in the internal sphincter muscle fibres.
- Straining due to constipation. This straining alone can push the cushions out of the anal canal and/or encourages congestion of the blood vessels. A high fibre diet can normally help prevent this cause of haemorrhoids.
- Pregnancy. The back-pressure caused by an increase in intra-abdominal pressure and associated dilation of blood vessels in the pelvic cavity are thought to encourage haemorrhoids.
With the underlying cause(s) still up for discussion, all haemorrhoids, however, present as a prolapse of the vascular and submucosal cushions, most commonly situated in the left lateral (outermost), right anterior (front) and right posterior (back) parts of the anal canal. These cushions are present from birth.
The Normal Anal Canal
The following diagram shows the normal anal canal. The pectinate (dentate) line divides than anus into the top two-thirds and lower third of the canal.
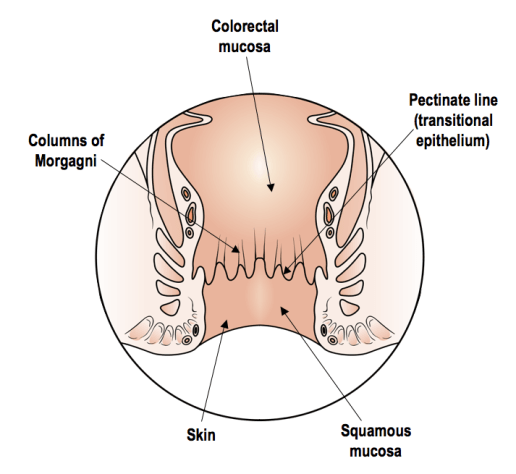
Normal anal canal. Haemorrhoids that originate above the pectinate line are called internal haemorrhoids, and those that originate below the line are external haemorrhoids. (Image adapted from wikicommons)
The Histology of a Haemorrhoid
The pectinate line can be identified histologically as the middle of the following three zones; the colorectal, transitional and squamous zones:
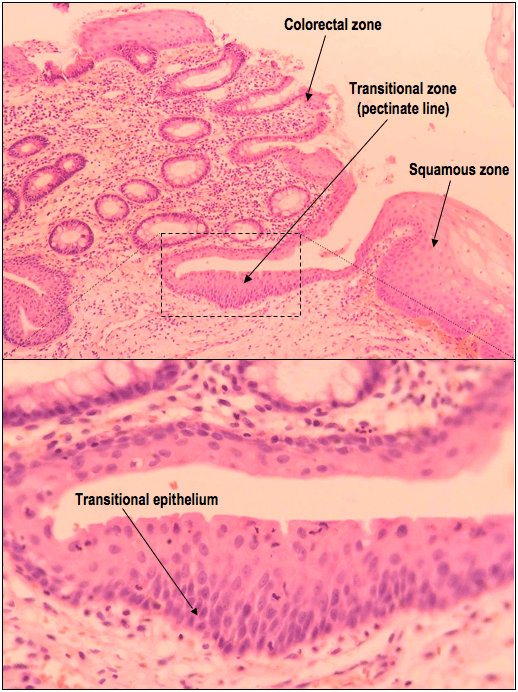
Upper: A low power H&E demonstrating the pectinate line, which is identified by the junction between the colorectal and squamous zones. Lower: A high power H&E of the transitional epithelium.
Haemorrhoids show very basic histology as they have just three main microscopic features:
- loose fibrovascular tissue at the submucosal level
- a collection of dilated (ectatic) blood vessels – often with more smooth muscle in their walls, so appear much thicker than regular veins. They may also show signs of thrombosis, too.
- lined by colorectal, transitional or squamous epithelium
Internal haemorrhoids are mostly lined by colorectal and transitional epithelium, but if they became very large they can be lined by all three. True external haemorrhoids are only lined my squamous epithelium. For an intriguing diagram that helps explain the different types of haemorrhoids, please see this informative webpage from Bupa.
So, now for some more histology:
A haemorrhoid lined by colorectal epithelium
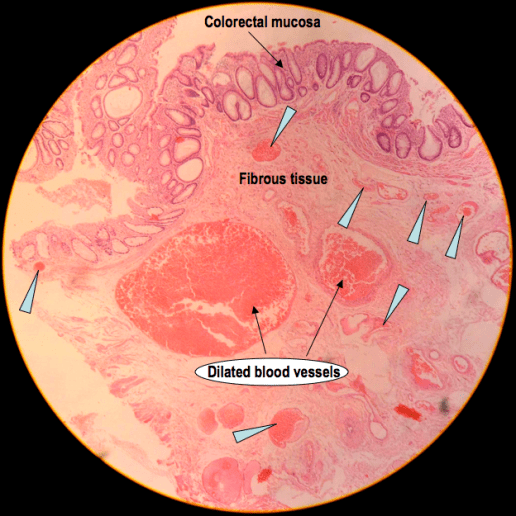
A high power H&E showing loose fibrovascular tissue (at the submucosal level) containing dilated blood vessels and lined by colorectal mucosa. There is also evidence of vascular proliferation (arrow heads)
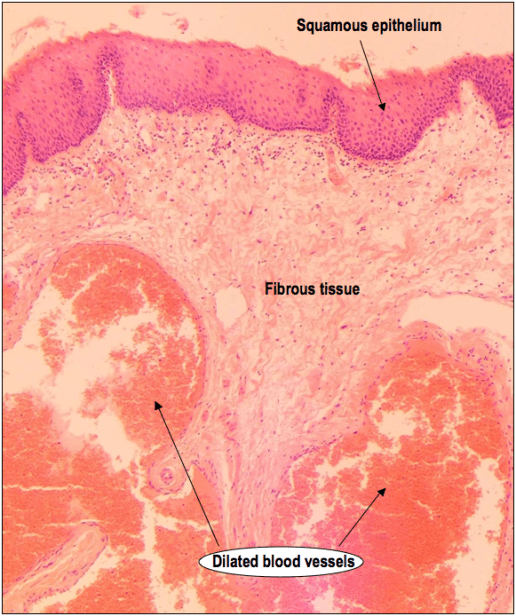
A haemorrhoid lined by squamous epithelium
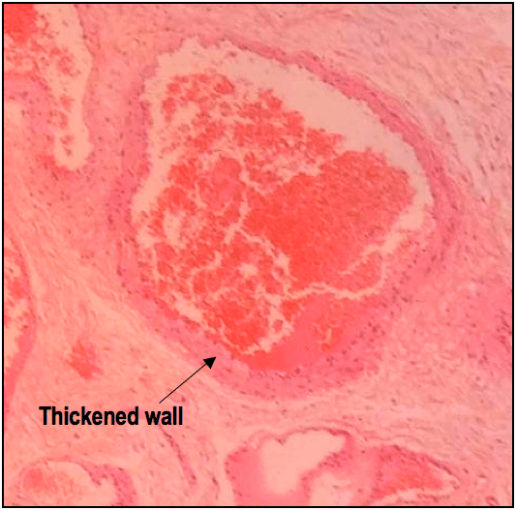
and now a close up of an ectatic vessel:
But can’t haemorrhoids be diagnosed clinically? Why bother doing histology on them at all?
This is a good question because, yes, haemorrhoids can be easily recognised with the naked eye. The reason why histology is recommended is because there are a number of other, more sinister, pathologies that could present in a similar way. Histology is required, therefore, to rule out these pathologies and prevent delayed misdiagnosis.
Some pathologies that macroscopically mimic haemorrhoids include:
- warts (condyloma, human papillomavirus [HPV])
- cytomegalovirus (CMV) infection
- hidradenoma papilliferum
- rectal cancer (a haemorrhoid may be its first presentation)
- anal duct carcinoma
- carcinoid
- lymphoma
- melanomas
So with just an idea of a few of the mimickers, it’s best to be properly sure!
All images are Copyright © 2014 Della Thomas.
**
Useful Links
For more information about haemorrhoids, including symptoms and treatments, please see here.
For more information about haemorrhoids during pregnancy, please see here.
Discussion
No comments yet.