Working in a histology lab means that I get to see a lot of what our body looks like under the microscope. Quarterly I will share with you some of my photos from the microscopic world of our inner space and tell you a little bit about what we’re looking at.
The tissue I have chosen to look at this quarter, you may be familiar with as the part that is tampered with when a man has a vasectomy. That part is called the vas deferens.
Removal of the vas deferens is a good surgical treatment for male sterilisation because it not only spares the release of male hormones from the testis into the bloodstream, its location and long length also allow for it to be easily found under the scrotal skin. This makes for a much simpler surgical technique and aftercare, with less scarring when compared to female sterilisation.Sperm’s Journey
Sperm are made in the testes but do not mature until they reach the epididymis (see diagram). Once mature and when the appropriate time comes, the vas deferens steps up to assist in the next stages of the sperm’s journey.
Although a minor role in sperm storage exists, the main role of the vas deferens is to carry sperm from the epididymis and deliver them to the ejaculatory duct. Here, they become mixed with fluid from the seminal vesicles and prostate before being expelled out of the body.
Putting all this into the context of the male urogenital system, if we zoom out from this first picture, the whole orientation looks a little something like this:
Extending from the tail of the epididymis, right up to the ejaculatory duct, the vas deferens averages at a staggering length of 30-40cm. It is a very narrow tube, with an average diameter of just 2-3mm, jam-packed full of muscle and blood vessels running through its entirety.
The muscle in the vas is mostly smooth muscle existing in hundreds of muscle fibres, organised into distinct layers around the lumen (the hole in the middle that runs the length of the vas and what the sperm travels through). This type of muscle is involuntary and only contracts under the influence from an external stimuli; which in this case is sexual arousal.
When the muscle fibres begin to contract, they propel the sperm upstream towards the ejaculatory duct. At this stage, the sperm is not completely motile and so this muscle motion is crucial for their transportation in their quest to win the race.
The orientation of the layers of muscle fibres are also crucial. Imagine a muscle fibre to be like a shoelace. Each layer of muscle around the lumen amounts to rows of hundreds of muscle fibres piled on top of each other, all bundled together like one big sheet of muscle. Now, one muscle sheet can be arranged so the fibres are laid out parallel to the length of the lumen and thus the whole length of the tube. These are called longitudinal muscle fibres. When they contract, they shorten and so are responsible for the shortening of the vas.
Other muscle fibres are arranged so that the individual fibres wrap around the circumference of the lumen to make a ring around it. These are called circular muscle fibres. When these contract and shorten, they are responsible for the constriction (and eventually widening, when they relax) of the diameter of the vas lumen.
The circular muscle fibres do not all contract simultaneously, instead they contract in waves along the length of the vas, much in the same way our food pipe (oesophagus) contracts when we swallow our food. This motion is called peristalsis, which is a bit like when you eat a freeze-pop and you push the ice lolly up to the open end of the wrapper whilst holding a pinch below it to prevent the ice lolly from dropping back down. The effect of these contraction waves also mean that whatever is being propelled forward, will continue in that direction regardless of gravity. This is why food will still enter your stomach even if you eat something when you are upside down.
So, now let’s see what this all looks like under the microscope:
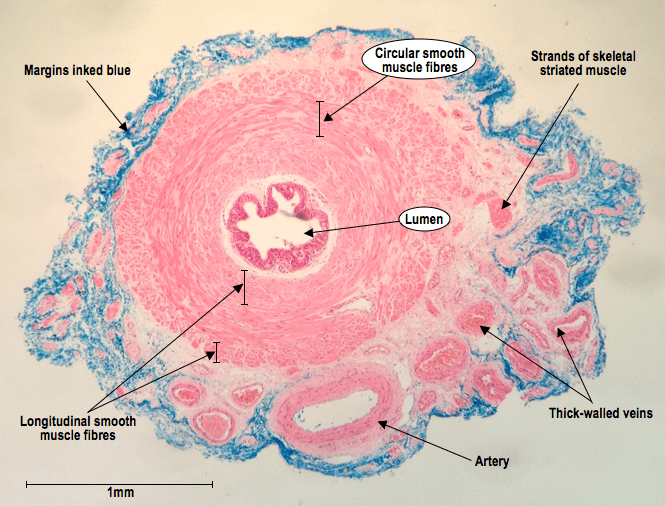
This is a section through the diameter of a vas deferens. The blue dye is just a marker of the margins that was painted on in the lab when the sample was being prepared. From this photomicrograph you get an idea of the extent of vascular supply. You can also see three distinct layers of muscle surrounding the lumen and the two different layouts they exist in.
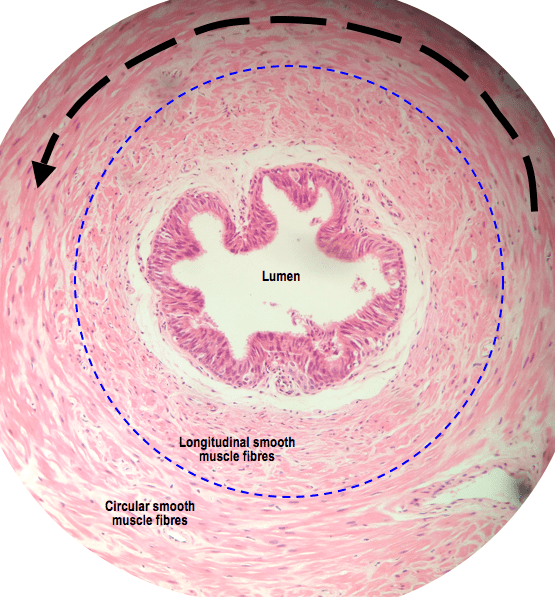
Here’s a closer look of the innermost and middle layer of smooth muscle:
All the muscle fibres are the same, it is just their orientation that gives them a different appearance when looking at them down the microscope. The circular muscle fibres, which wrap around the circumference of the vas, have a distinctive spindly looking appearance and the nuclei appear elongated. Imagining those shoelaces again to help explain this; visualise wrapping (arched arrow, above) those laces around a toilet roll inner and then taking a bread slice across the diameter of the tube, including the shoelace. The appearance of the laces would be long and spiral shaped, only exposing the horizontal edge of possibly just one lace.
A section through the longitudinal muscle fibres has a distinctive look also. These muscle fibres appear more rounded, as do their nuclei, and this is because the section is like looking down on a slice through the top of multiple vertically stacked fibres. This would expose multiple fibres, showing the full width of their diameter.
In the following diagram (using cardiac muscle to explain), the inner- and outer-most muscle fibres (from my photomicrograph) are represented by the red slice, and the middle layer is represented by the blue slice.
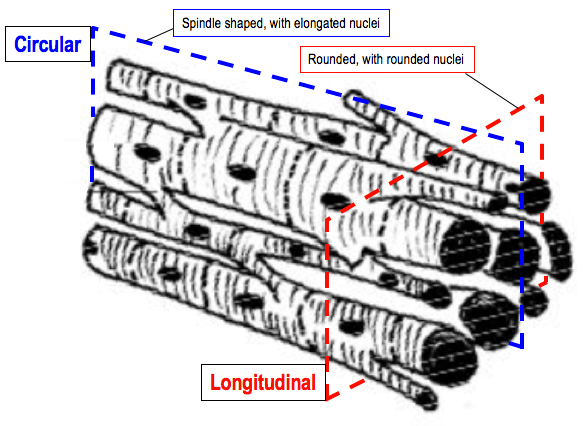
Why the same muscle fibres look differently, depending on their orientation in the section. [credit/adapted: wikicommons]
The lumen of the vas is very interesting.
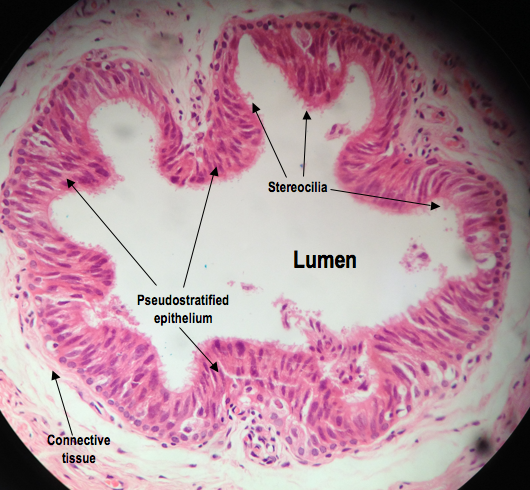
It is lined with what is known as pseudostratified epithelium. The name “stratified epithelium“ describes a lining that consists of multiple layers of epithelium, meaning that only one layer is in contact with the basal lamina (like how a brick wall only has its first level in contact with the floor). Stratified epithelium is easily spotted because you can see nuclei at varying distances from the first layer of the lining, which indicates multiple layers. In “pseudostratified” (“pseudo” from a Greek word meaning “false”) epithelium, however, the nuclei look like they may also be in different layers, but in actual fact the lining is only one layer thick. All cells in pseudostratified epithelium touch the basal lamina, it is just the shape of the cells and positioning of the nuclei that suggest otherwise.
After a vasectomy, where does the sperm go?
A man can produce millions of sperm everyday. Not all of these become expelled, and yes that may be obvious for men who have had a vasectomy, but this is also true for men who haven’t. So, they literally just accumulate in the epididymis and vas deferens.
In order to prevent these stragglers from causing any obstruction, the body reabsorbs them, and pseudostratified epithelia are great absorbers so are perfect for the job. The efficiency of their reabsorption is enhanced by both the tiny extensions of their cell membrane, known as stereocilia (as labelled above), and the undulated vas lining; both of which help increase its surface area. The name “stereocilia” is a little misleading because “cilia” implies motility, but these stereocilia do not move and so they are more like the tiny microvilli that are found in the gut. They are also found in the epididymis, which is useful because absorption needs to be optimised here also as many sperm fail to leave the epididymis, too.
When sperm are reabsorbed by the epithelium, immune cells known as macrophages engulf, digest and dispose of them like they routinely do with any other cell debris or bacterium lying around, unwanted by the body. This is a completely normal and routine process. The only difference between men who have had a vasectomy and those who haven’t, is that the epithelial cells need an extra hand with reabsorbing the sperm and so the number of macrophages increase in that area. Sperm only accounts for a very small percentage of the total volume of ejaculate (about 5%), therefore, after a vasectomy there’s no need to worry about suffering from swollen sacs, the additional macrophages will have no problems handling the situation.
Other features and why testicles appear to shrink in the cold:
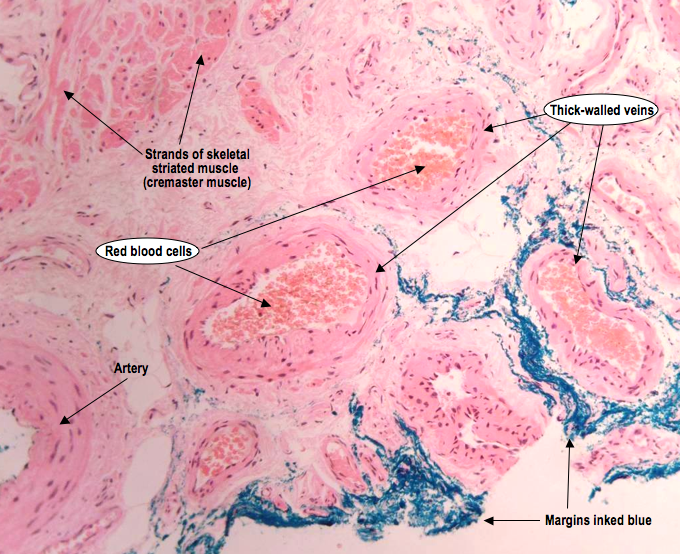
This photomicrograph takes a closer look at the blood supply. The veins in the testes are uncharacteristically thick-walled, making them sometimes difficult to distinguish from arteries. They can often be identified as those with a wider lumen, but most of the time it just needs good experience. The red blood cells are also a lot clearer to identify at this magnification.
So, I mentioned something about shrinking testicles….
Well, this can be explained by another interesting feature seen in this image called the cremaster muscle (heck, it even has its own Facebook page). This muscle is responsible for the raising and lowering of the testicles; the direction of which is dependent on the circumstance. Its ultimate goal is to provide optimal conditions for the production of sperm (spermatogenesis), which is around 2°C below body temperature (so about 35°C). When air or body temperature drops, the cremaster muscles contract to raise the testes and draw them closer to the body for extra warmth. Alternatively, when temperatures rise, the cremaster muscles relax and the testes are lowered into a position further away from the body to try to cool them down. As you can see, any sudden temperature drops such as those caused by jumping into a cold swimming pool, would cause rapid cremasteric contractions that quickly pull the testes closer to the body in an attempt to keep them as warm as possible.
Why are vasectomy samples sent to a pathology lab?
It’s a good question because most tissue samples are sent to a pathology lab to look for signs of disease. It’s just as crucial that the resected vas deferens are also sent for analysis to confirm that the removed sample is indeed a vas deferens and not anything else, such as a nerve for example. It is also imperative that, post-vasectomy, the man provides repeat semen samples for analysis a few weeks later to confirm the procedure has worked. Only when given the all-clear from a healthcare professional can the vasectomy be relied on as a form of contraception.
References and useful links:
How sperm are re-absorbed into the body
Fundamentals of Anatomy & Physiology 5th Edition. Martini et al.
For more information and advice on vasectomy and if it’s right for you and your partner, here are some useful links:
All images are Copyright © 2012 Della Thomas, unless otherwise stated.


Discussion
No comments yet.